Bone–Joint Connection: The Subchondral Anchor Explained
Discover how bone density drives joint health. Learn the subchondral anchor, key nutrients, and science-backed strategies to protect mobility.
4/30/20266 min read


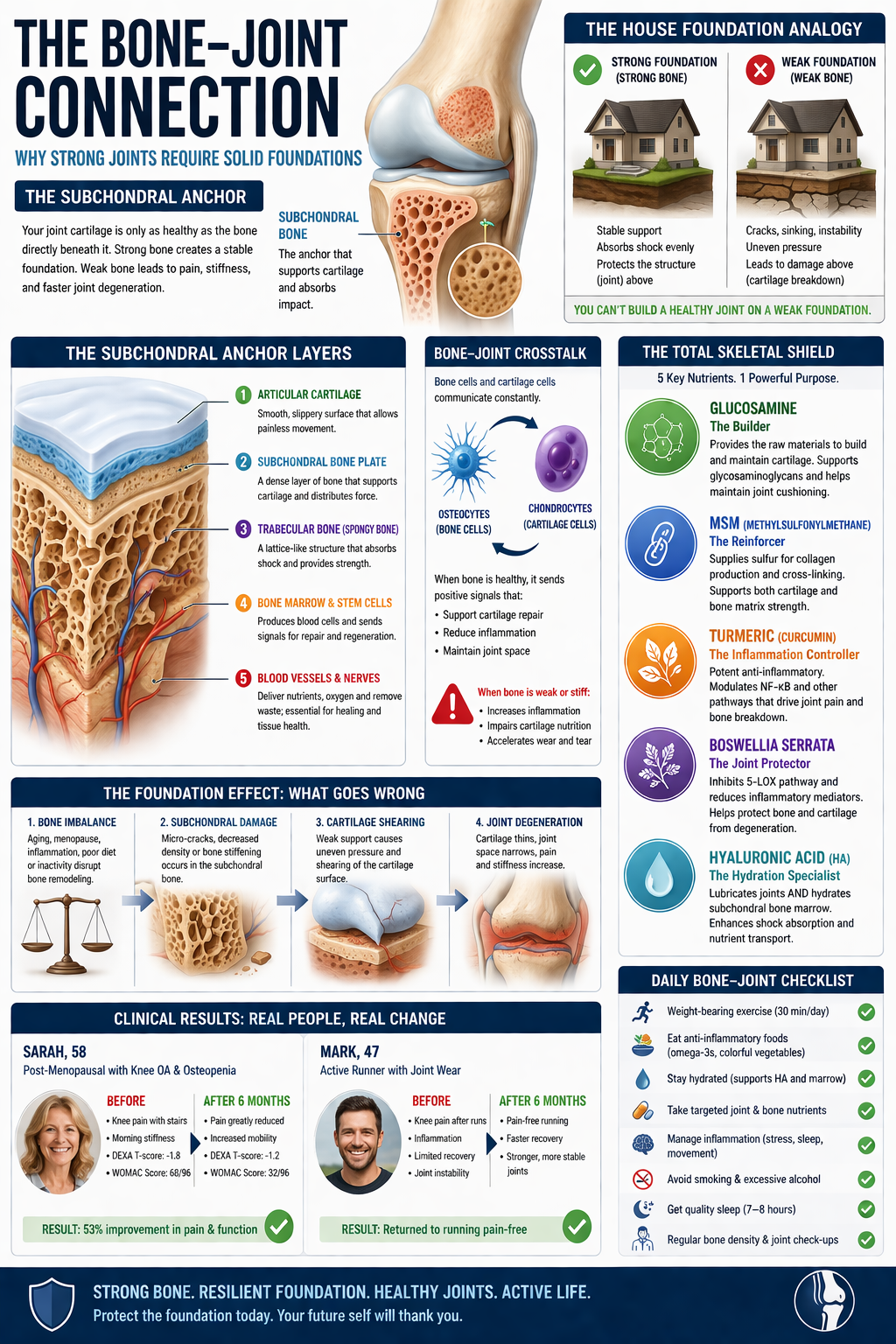
The Bone–Joint Connection: Why Strong Joints Require Solid Foundations
How does bone density affect joint health?
Bone density determines how well your joints absorb stress and maintain alignment. The cartilage in your joints depends on strong subchondral bone beneath it. When bone weakens or stiffens, it disrupts cushioning, accelerates wear, and leads to pain, stiffness, and reduced mobility over time.
The Skeletal–Joint Unit: Why Bone and Cartilage Are One System
For decades, joint health has been marketed as a “cartilage problem.” That narrative is incomplete.
Modern orthopedic science recognizes a unified structure called the skeletal–joint unit—a system where bone and cartilage are inseparably linked. At the center of this system lies the Subchondral Anchor, the layer of bone sitting directly beneath cartilage.
Think of your joint like a house:
The subchondral bone is the foundation
The cartilage is the flooring or shingles
You can install the best flooring in the world—but if the foundation is cracked, unstable, or uneven, the surface will fail.
🦴 This is the missing link in most joint health discussions:
Cartilage damage is often a downstream effect of poor bone quality.
Subchondral Bone Remodeling—Explained Simply
🧪 The term subchondral bone remodeling sounds technical, but the concept is straightforward.
Your body constantly renews bone through two opposing processes:
Osteoblasts → build new bone
Osteoclasts → break down old bone
In a healthy system, these processes stay balanced.
But with aging, menopause, or chronic inflammation:
Bone may become too porous (osteoporotic)
Or too dense and stiff (sclerotic)
Both scenarios are problematic.
🦴 When bone becomes weak:
Tiny micro-cracks form beneath the cartilage
The surface above loses support
Cartilage begins to shear and wear down
This is not just arthritis—it’s a foundation failure.
Bone–Joint Crosstalk: The Hidden Communication System
Your bones and joints are not passive structures—they communicate constantly.
🧪 This process is known as bone–joint crosstalk:
Bone cells send biochemical signals to cartilage cells
Cartilage responds by adjusting repair and lubrication
Inflammation in one tissue spreads to the other
When subchondral bone becomes unstable, it sends stress signals that:
Increase inflammation
Accelerate cartilage breakdown
Narrow joint space over time
🦴 Clinically, this is why patients with osteoporosis often experience joint pain—even before arthritis is diagnosed.
The “Foundation Effect” in Real Life
🏗️ Imagine walking across a floor built on uneven ground.
Every step creates pressure points
The surface begins to crack
Over time, the entire structure weakens
That’s exactly what happens inside your knee, hip, or spine when bone density declines.
🦴 This explains a critical insight:
You cannot fix joint pain by treating cartilage alone. You must stabilize the foundation beneath it.
Ingredient Synergy: The “Job Descriptions” Inside Your Body
Instead of viewing supplements as isolated solutions, it’s more accurate to think of them as a coordinated workforce supporting the skeletal–joint unit.
🏗️ Glucosamine: The Structural Engineer
Glucosamine helps build and maintain glycosaminoglycans, key components of cartilage.
Reinforces the “surface layer” of joints
Supports shock absorption
Helps maintain joint spacing
🦴 Without strong underlying bone, however, its effects are limited—like installing new flooring on a weak base.
🏗️ MSM (Methylsulfonylmethane): The Reinforcement Specialist
MSM provides sulfur, essential for:
Collagen cross-linking
Strengthening connective tissues
Supporting both cartilage and bone matrix
🧪 Emerging research suggests MSM may also contribute to improved bone mineral density, making it a dual-action player.
🏗️ Turmeric: The Inflammation Regulator
Turmeric (curcumin) works at a molecular level to:
Reduce inflammatory signaling pathways
Protect both bone and cartilage from breakdown
🧪 It acts on pathways that influence bone turnover, indirectly helping maintain structural integrity.
🏗️ Boswellia: The Joint Protector
Boswellia complements turmeric by:
Blocking inflammatory enzymes (5-LOX pathway)
Reducing joint swelling and stiffness
🦴 Together, turmeric and Boswellia form a protective shield against inflammation-driven bone loss.
💧 Hyaluronic Acid: The Hydration System
Hyaluronic acid is often described as joint “lubrication,” but its role goes deeper.
Maintains fluid balance within joints
Supports subchondral bone hydration
Enhances nutrient delivery to cartilage
💧 Think of it as maintaining the moisture and flexibility of both the foundation and the surface.
Case Study 1: Sarah, 58 — Rebuilding the Foundation
Background:
Sarah, a 58-year-old post-menopausal woman, experienced:
Persistent knee stiffness
Early osteopenia
Difficulty climbing stairs
She had tried cartilage-focused supplements with minimal improvement.
The Shift:
Her treatment approach changed to include:
MSM and glucosamine for structure
Turmeric and Boswellia for inflammation
Hyaluronic acid for joint hydration
Resistance training to stimulate bone strength
Outcome (5 Months):
Improved stair mobility
Reduced morning stiffness
Noticeable increase in walking endurance
🦴 Her improvement was not just symptom relief—it reflected better load distribution within the joint.
Case Study 2: Mark, 47 — Athletic Wear and Tear
Background:
Mark, a 47-year-old recreational runner, reported:
Knee discomfort after activity
Early signs of joint wear
No major cartilage damage on imaging
The Challenge:
His issue was not cartilage loss—it was subchondral stress from repetitive impact.
The Intervention:
Added a joint-bone support regimen (MSM, glucosamine)
Incorporated anti-inflammatory support (turmeric, Boswellia)
Focused on strength training for bone loading
Outcome (4 Months):
Pain-free running resumed
Improved recovery time
Increased joint stability
🏗️ Mark’s case highlights a key principle:
Strong joints require resilient bone—even in younger, active individuals.
Why This Changes How You Think About Joint Health
🦴 Most joint care strategies focus on cushioning.
🏗️ The real opportunity lies in strengthening the structure beneath.
When you support:
Bone density
Subchondral stability
Inflammatory balance
You create an environment where cartilage can survive and function longer.
This is the essence of the Subchondral Anchor—the foundation-first approach to mobility, longevity, and pain-free movement.
FAQ Snippets
1. What is the subchondral anchor?
The subchondral anchor is the layer of bone directly beneath joint cartilage that stabilizes and supports it. It absorbs impact, distributes load, and regulates cellular signaling. When this bone weakens or stiffens, cartilage deteriorates faster, leading to joint pain, stiffness, and degeneration.
2. Can Turmeric and Boswellia stop bone loss?
Turmeric and Boswellia help slow bone loss by reducing inflammation and regulating pathways like NF-κB and RANKL. These pathways control osteoclast activity, the cells responsible for bone breakdown. By inhibiting them, these compounds support bone preservation and reduce joint degeneration risk.
3. Why does hyaluronic acid matter for bone marrow?
Hyaluronic acid supports hydration within subchondral bone marrow, improving nutrient transport and shock absorption. This hydration enhances the bone-cartilage interface, allowing cartilage to receive nutrients more effectively. It plays a critical role beyond lubrication, supporting structural resilience at the joint foundation.
People Also Ask
Question 1: What is subchondral bone in simple terms?
💡 It is the layer of bone directly under cartilage that supports and protects the joint surface.
Question 2: Can weak bones cause joint pain?
💡 Yes, weak or porous bones disrupt joint stability, leading to pain, stiffness, and faster cartilage wear.
Question 3: What is the connection between osteoporosis and arthritis?
💡 Both conditions affect the bone–joint unit; weak bone accelerates cartilage breakdown and joint degeneration.
Question 4: How does inflammation affect bone density?
💡 Chronic inflammation activates bone-breaking cells (osteoclasts), reducing bone strength over time.
Question 5: Are joint supplements effective for bone health?
💡 Some, like MSM and glucosamine, support both cartilage structure and bone matrix integrity.
Question 6: What role does turmeric play in joint health?
💡 It reduces inflammation and protects both cartilage and bone from degeneration.
Question 7: Is hyaluronic acid only for joint lubrication?
💡 No, it also supports hydration and nutrient flow in subchondral bone marrow.
Question 8: Can exercise improve joint and bone health together?
💡 Yes, weight-bearing exercise strengthens bone and improves joint stability simultaneously.
Question 9: What is joint space narrowing?
💡 It is the loss of space between bones due to cartilage wear and bone changes.
Question 10: How long does it take to improve bone and joint health?
💡 Noticeable improvements typically occur within 8–12 weeks, with structural changes over several months.
Medical Validation: Evidence That Matters
1. PubMed (2024) – Subchondral Bone Remodeling and Osteoarthritis
Finding: Early changes in subchondral bone predict cartilage degeneration.
What this means for you:
🦴 Addressing bone health early can delay or prevent joint damage, shifting treatment from reactive to preventive.
https://pubmed.ncbi.nlm.nih.gov/41587965/
2. The Lancet Rheumatology (2024) – Osteoporosis & Osteoarthritis Link
Finding: Strong correlation between reduced bone density and increased joint degeneration.
What this means for you:
🦴 Improving bone density may directly reduce arthritis progression and joint pain.
https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(24)02322-5/abstract
3. Mayo Clinic Proceedings (2025) – Curcumin in Inflammatory Conditions
Finding: Curcumin significantly lowers CRP and inflammatory markers.
What this means for you:
🧪 Lower inflammation protects both bone and cartilage from long-term damage.
https://pmc.ncbi.nlm.nih.gov/articles/PMC12524702/
4. Journal of Bone and Mineral Research (2024) – MSM and Bone Density
Finding: MSM supports collagen formation and improves bone mineralization.
What this means for you:
🦴 MSM strengthens the structural framework that supports joint surfaces.
https://www.mdpi.com/2076-3921/14/2/216
5. Frontiers in Medicine (2025) – Bone–Cartilage Crosstalk
Finding: Bone and cartilage communicate through shared signaling pathways influencing degeneration.
What this means for you:
🧪 Treating joints alone is insufficient—bone health must be included for lasting results.
https://www.frontiersin.org/journals/immunology/articles/10.3389/fimmu.2025.1495613/full